
How Housing Makes a Difference in Our Health
Access to safe, stable housing serves as a key foundational component for our health and well-being – in fact, so

Access to safe, stable housing serves as a key foundational component for our health and well-being – in fact, so

High blood pressure can increase your risk for stroke, heart failure, heart disease, and other life-threatening conditions. Here are six

The weeks following birth can be exciting, stressful, and filled with questions. No matter your future family plans, postpartum birth

Statin therapy is often used to treat high cholesterol and help prevent cardiovascular disease, but many people have questions about
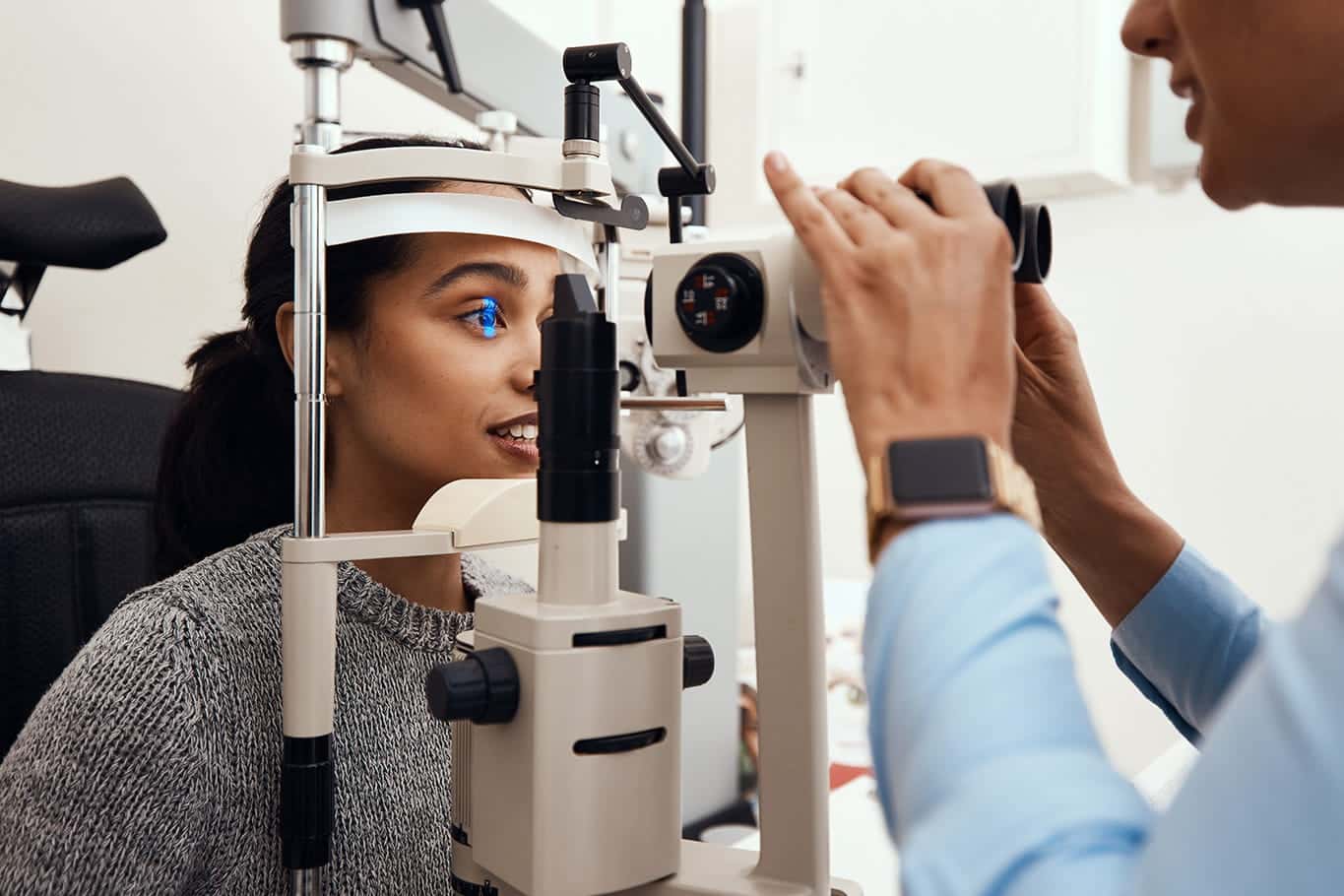
Regular eye exams are key to maintaining your vision health. Learn how often you should get an eye exam and
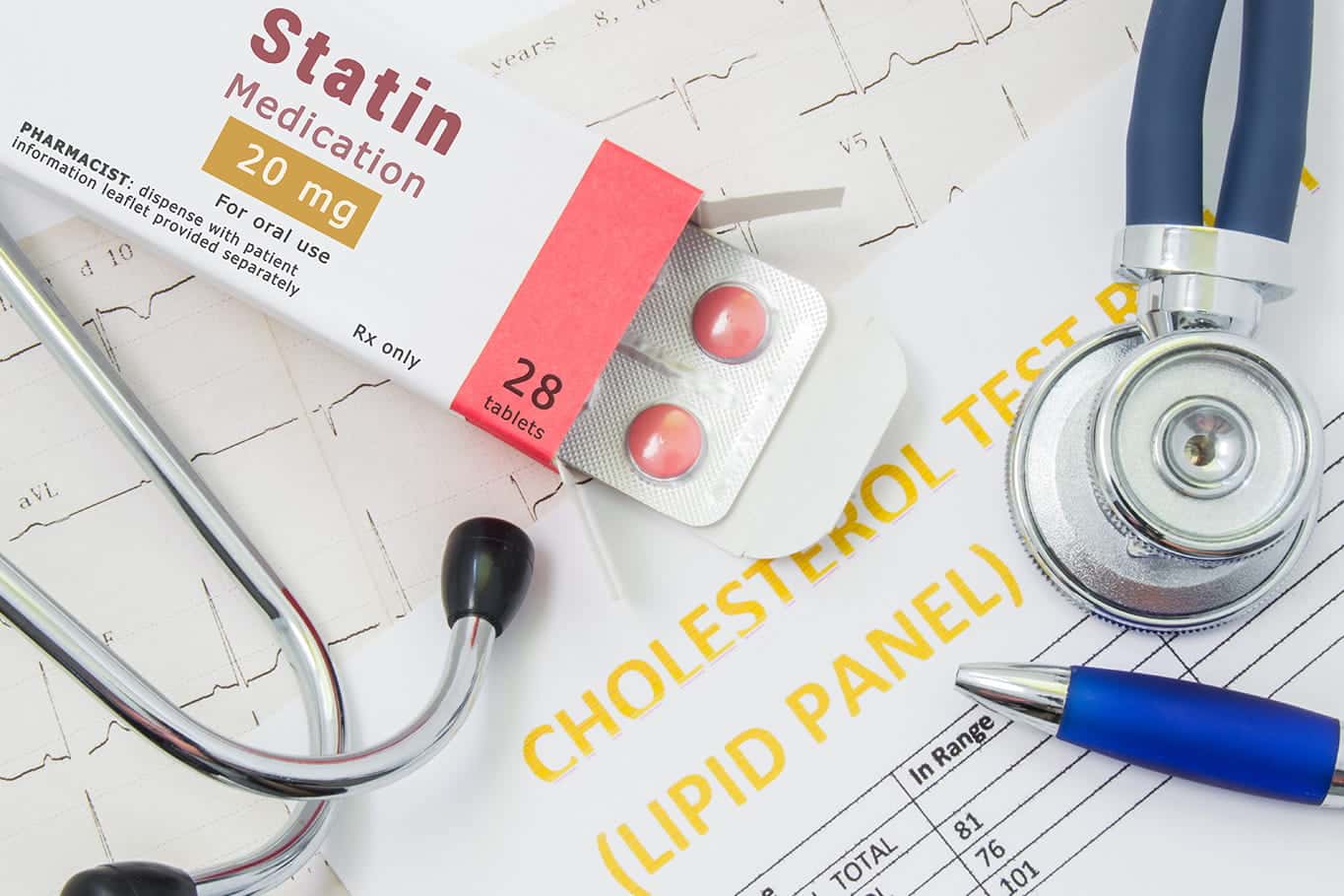
The American Diabetes Association (ADA) recommends statin therapy for most adults with diabetes based on their risk of cardiovascular disease,
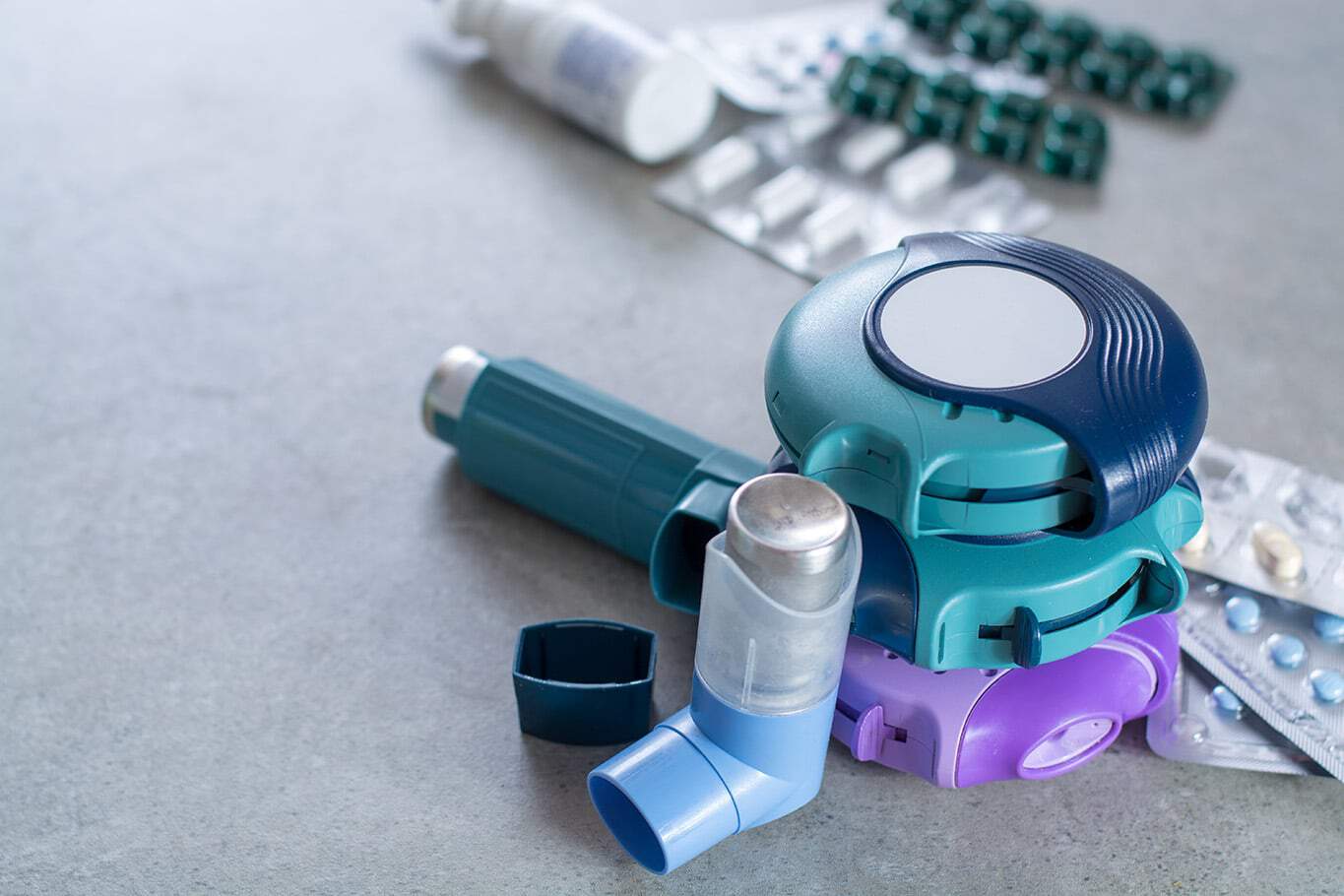
Following your asthma medication schedule is vital to managing the condition. Here’s what you need to know.

Chronic kidney disease affects approximately one out of every three individuals with diabetes. Here’s how to improve kidney health, including

Antidepressants are prescription medications used to treat depression. There are many types of antidepressants, and they all work in different

Behavioral health and mental health are closely related, but there are some unique differences between the two. Find out why

Sexually transmitted diseases (STDs) are common, particularly among teens and young adults ages 15-24. Take steps to protect your health

Colorectal cancer is cancer that begins in the colon or rectum. Here’s what you need to know about colorectal cancer

Aging is inevitable and can affect many families. Here are tips for caring for elderly parents while keeping your self-care

Oral health plays an essential role in your overall health and well-being. Here’s what you need to know about how

Knowing where to go when you need care is so important. Learn how seeking help at an urgent care clinic

Aside from skin cancers, breast cancer is the most common form of cancer in U.S. women. Watch for these early

All food we eat contains macronutrients and micronutrients. Read about what they are, why they matter, and how to make

Grand Junction is a lively town in Colorado’s Grand Valley and a fantastic place to live. Learn more about the